How Caregiver Scheduling Software Supports Clinician Work-Life Balance and Retention
Workforce shortages remain one of the most significant barriers to expanding access to home-based care. Across home health, hospice, and personal care, agencies are facing rising patient demand while competing for a limited pool of clinicians and caregivers.
While compensation and hiring strategies often dominate workforce discussions, schedule stability and work-life balance increasingly determine whether clinicians stay or leave an organization.
Predictable schedules, manageable workloads, and reduced administrative burden play a critical role in clinician satisfaction. As a result, many organizations are rethinking how caregiver scheduling software and healthcare software systems can support both workforce sustainability and patient care delivery.
Why Work-Life Balance Matters More Than Ever
The healthcare workforce continues to experience unprecedented strain. Data from the CDC highlights just how widespread these challenges have become.
- 46% of health workers reported often feeling burned out in 2022, up from 32% in 2018.
- 44% reported they intended to look for a new job, compared with 33% in 2018.
- More than twice as many health workers reported workplace harassment in 2022 compared to 2018.
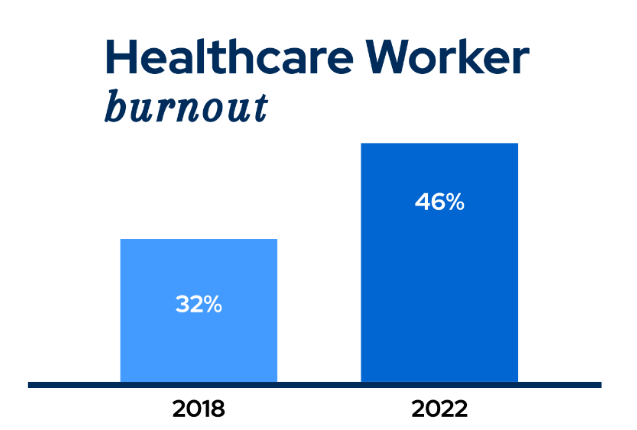
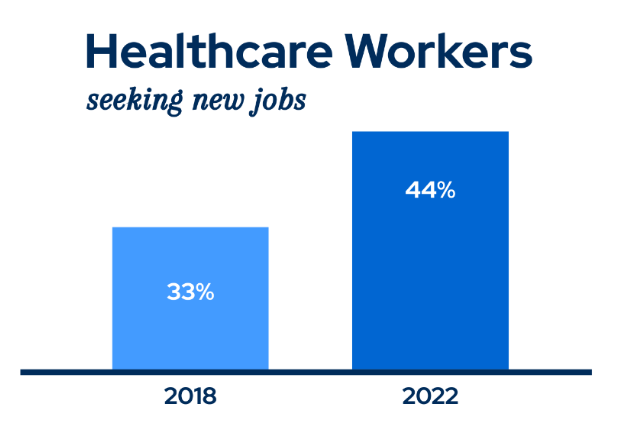

These statistics highlight a troubling trend: many healthcare professionals feel overwhelmed, unsupported, or disengaged from their work environments.
For home-based care organizations, burnout can be especially challenging because clinicians spend much of their time in the field. Without stable schedules and efficient operational support, clinicians often experience:
- Long or unpredictable workdays
- Excessive travel between visits
- Administrative work after hours
- Frequent schedule changes
Over time, these issues contribute to fatigue, job dissatisfaction, and higher turnover.
The Scheduling Challenge in Home-Based Care
Scheduling in home-based care is inherently complex. Each patient visit must account for numerous factors, including:
- Clinician licensure and skill mix
- Geographic location and drive time
- Patient preferences and availability
- Productivity expectations
- Continuity of care requirements
In many agencies, these factors are still managed through manual scheduling processes that rely heavily on individual schedulers’ experience. While this approach can work for smaller organizations, it becomes difficult to maintain as patient volume increases and service lines expand.
Common operational challenges include:
- Schedules finalized late in the day
- Frequent last-minute visit changes
- Inefficient routing that increases drive time
- Missed visits or delayed starts of care
- Increased after-hours communication with clinicians
For clinicians, these disruptions often translate into longer workdays and less control over their schedules.
The Link Between Scheduling and Clinician Retention
When schedules are unpredictable or constantly changing, clinicians absorb the impact.
Unstable schedules can lead to:
- Increased stress and burnout
- Difficulty balancing work and personal life
- Reduced job satisfaction
- Higher turnover rates
Conversely, agencies that prioritize predictable scheduling often see improvements in both clinician satisfaction and retention.
Providing clinicians with earlier schedule visibility, balanced workloads, and optimized routes can significantly improve day-to-day working conditions.
This is where caregiver scheduling software can play a valuable role.
How Caregiver Scheduling Software Improves Work-Life Balance
Modern patient scheduling and caregiver scheduling software helps agencies move beyond manual coordination toward more efficient and predictable workforce management. Instead of building schedules one visit at a time, scheduling platforms use configurable rules and automation to support decision-making. Key scheduling software features often include:
Advanced Visit Planning – Automated tools can assign visits based on clinician skills, patient needs, and geographic proximity.
Route Optimization – Scheduling systems can reduce unnecessary travel by organizing visits in a more efficient order.
Schedule Predictability – Schedules can be created days or weeks in advance, giving clinicians greater visibility into upcoming workloads.
Workload Balancing – Automation can distribute visits evenly across clinicians, helping prevent burnout and excessive overtime.
Together, these capabilities allow agencies to maintain operational efficiency while improving clinician experience.
Why Scheduling Is Becoming a Technology Priority
As workforce challenges intensify, many healthcare organizations are turning to technology to reduce administrative burdens and improve workforce management.
Industry research reflects this growing focus. In a recent Home Health Care News Outlook Survey, 31% of participating leaders identified scheduling as the operational area most likely to benefit from artificial intelligence.
This insight highlights how scheduling has evolved from a back-office task into a strategic operational capability. Organizations are increasingly exploring AI-driven tools and automation within healthcare software systems to help manage workforce complexity while maintaining quality care.
By automating routine scheduling tasks, agencies can allow schedulers and clinical leaders to focus on higher-value activities such as workforce planning and patient coordination.
The Operational Benefits of Scheduling Optimization
Improved scheduling processes do more than support clinician work-life balance. They can also help agencies operate more efficiently. When schedules are optimized, agencies may see improvements in:
- Timely start of care
- Visit completion rates
- Continuity of care
- Clinician productivity
- Reduced missed visits
Additionally, optimized scheduling can help agencies better understand workforce capacity, making it easier to accept referrals and serve more patients.
In an environment where workforce shortages limit growth, maximizing the efficiency of existing staff becomes a key strategic advantage.
A Strategic Approach to Workforce Sustainability
Addressing clinician burnout requires more than a single operational improvement. However, scheduling plays a central role in shaping the daily experience of field clinicians. Organizations seeking to improve clinician satisfaction and retention can start by evaluating:
- Average drive time per clinician
- Visit distribution across the week
- Frequency of schedule changes
- After-hours documentation and communication
- Clinician workload variability
From there, agencies can explore ways to standardize scheduling workflows and leverage modern caregiver scheduling software to support more predictable schedules. Even incremental improvements in scheduling stability can help clinicians feel more supported and empowered in their roles.
Supporting the Future of Home-Based Care
Demand for home-based care will continue to rise as the population ages and healthcare systems shift more services into the home. At the same time, workforce shortages and burnout threaten the industry’s ability to meet that demand.
By prioritizing clinician experience and investing in smarter operational systems, including modern patient scheduling tools, agencies can build a more sustainable workforce model.
Predictable schedules, reduced administrative burdens, and improved workflow efficiency help clinicians focus on what matters most: delivering high-quality care to patients in their homes. For agencies navigating today’s workforce challenges, optimizing scheduling may be one of the most practical, and impactful, steps they can take. Start a conversation with our team to find out how HCHB can help your agency optimize scheduling.










