Revenue cycle management in healthcare (RCM) is the process of managing the financial lifecycle of patient care from initial referral and eligibility verification through claim submission, reimbursement, and accounts receivable resolution.
In home health and hospice, RCM connects clinical care delivery to financial outcomes. Every step, from documentation to billing directly impacts whether organizations are reimbursed accurately and on time.
At its core, effective RCM ensures that:
- Services provided are accurately documented and billable
- Claims are submitted correctly the first time
- Payments are collected efficiently and predictably
For executive leaders, RCM is not just a back-office function. It is a primary driver of cash flow, margin protection, and financial stability.
Why revenue cycle management matters more now
Home-based care organizations are operating in an increasingly complex reimbursement environment. Across both home health and hospice, leaders are navigating:
- Rising healthcare claims denial management complexity, particularly with Medicare Advantage and commercial payers
- Ongoing staffing constraints impacting billing, intake, and authorization workflows
- Increased need for real-time financial visibility
- Regulatory requirements that tie documentation quality to reimbursement
These pressures mean that improving revenue cycle management is no longer optional, it is essential to sustaining operations and enabling growth.
The key stages of the healthcare revenue cycle
Understanding the full revenue cycle is critical to identifying where performance breaks down.
1. Referral, intake, and eligibility verification
The cycle begins before care delivery. Accurate patient information, insurance verification, and authorization processes establish the foundation for clean claims.
2. Clinical documentation and coding
Documentation must fully support the services delivered and meet payer requirements. Incomplete or inconsistent documentation can delay or prevent reimbursement.
3. Charge capture and claim submission
Claims must be generated accurately and submitted promptly. Errors at this stage often lead to rework, delays, and denials.
4. Payment processing and reimbursement
Payers adjudicate claims and issue payments. Variability across payers can impact both timing and reimbursement levels.
5. Accounts receivable (AR) management
Outstanding claims must be actively managed to ensure timely resolution and prevent revenue leakage.
6. Denial management and appeals
Denied claims require investigation, correction, and resubmission. A proactive approach to healthcare claims denial management reduces repeat issues.
Where revenue cycle performance breaks down
Even well-run organizations experience friction across the revenue cycle. Common breakdowns include:
- Incomplete intake and authorization workflows leading to avoidable denials
- Documentation gaps that prevent claims from being billed or paid
- Low first-pass clean claim rates, increasing rework and delays
- Limited visibility into AR and payer performance
- Staffing gaps that slow billing and collections
For many organizations, these issues compound, creating longer DSO, increased write-offs, and reduced financial predictability.
What strong revenue cycle performance looks like
Organizations that successfully improve revenue cycle management tend to demonstrate consistent performance across key metrics.
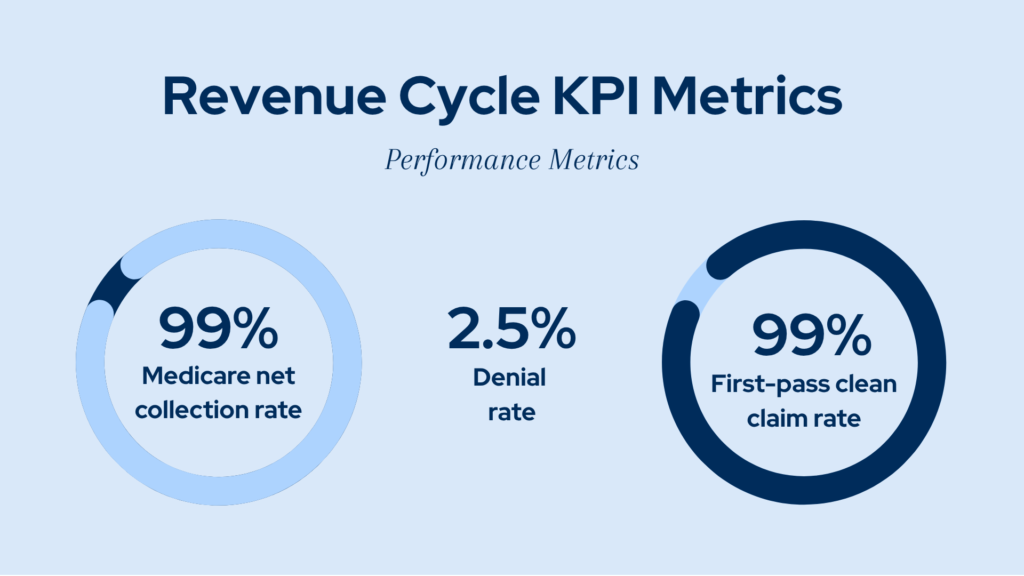
For example, structured revenue cycle approaches have achieved:
- 99% first-pass clean claim rates
- 2.5% denial rates
- 99% Medicare net collection rates
These outcomes are directional and depend on organizational context, but they reflect the impact of aligned processes, expertise, and operational discipline.